Antibiotics: Function, Bacterial Interaction & Antibiotic Resistance
Edited by Jamie (ScienceAid Editor), XanthousOfTheThirdQuadrant, Jen Moreau, Sim and 2 others
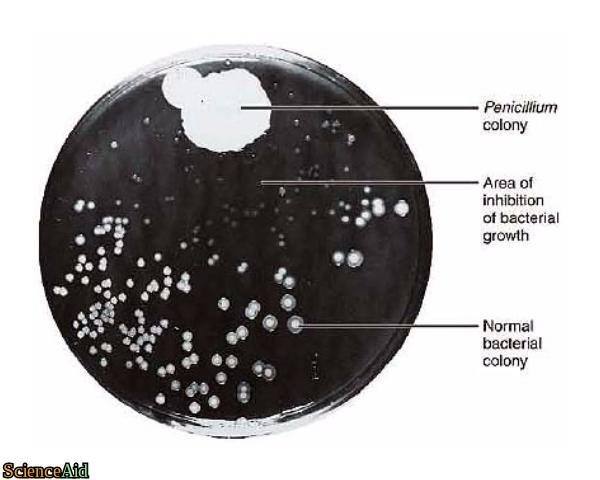
Antibiotics are potent antimicrobials that are used in the treatment of bacterial infections. Antibiotics are ineffective in the treatment of viruses such as colds and cases of flu. It might be difficult to believe, but antibiotics were only fully discovered and developed less than 100 years ago, 89 to be exact. Penicillin, the first antibiotic was discovered in 1928 by Sir Alexander Fleming, a Scottish scientist, and botanist who discovered Penicillin, a genus of fungi produced antimicrobial properties. Fleming went on to discern that penicillin could be utilized as an antibiotic to treat illnesses and sicknesses that were catastrophic prior to his discovery including pneumonia, syphilis, meningitis, typhoid fever and tuberculosis
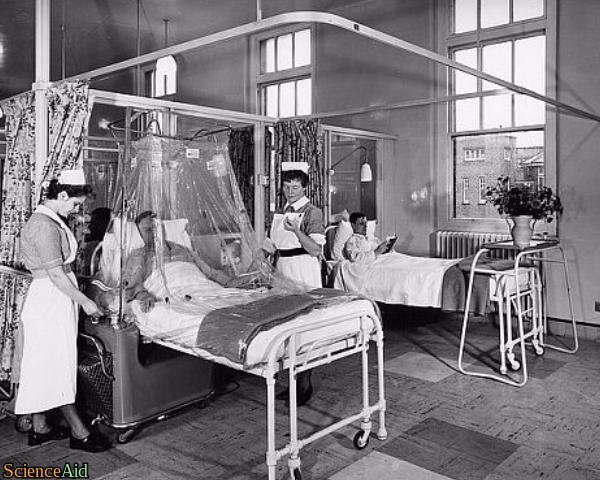
Although discovered before the outbreak of the war, it was World War II that really popularized penicillin pushing it into the mainstream as a revolutionary treatment reducing the number of war amputations and casualties. Penicillin was proven so effective during the war that production increased to 650 billion units produced in 1945 from a modest 400 million in 1943 [1].The discovery and effectiveness of penicillin, the progressive invention of other antibiotics in conjunction with the discovery and usage of vaccinations have eradicated many diseases that in the past were devastatingly calamitous
.
Antibiotics: Function and Bacterial Interaction
Antibiotics work effectively by killing bacterial microorganisms, referred to as bactericidal; or by inhibiting the growth of bacterial microorganisms, referred to as bacteriostatic.
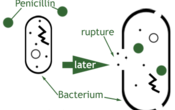
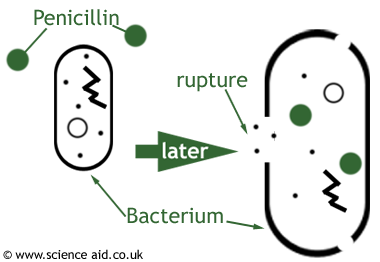
Penicillin is an example of a bactericidal antibiotic and acts by killing bacteria cells. Penicillin is able to differentiate between healthy human cells and bacteria cells because many bacteria cells have cell walls while human cells do not have cell walls. The cells walls in bacteria are termed cell wall: peptidoglycan. The peptidoglycan builds powerful walls around the bacteria to protect them and deter extrinsic matter or particles to enter them. Penicillin is able to inadvertently destroy peptidoglycan during cell division. When the bacteria cells divide, small holes open up in the peptidoglycan during division, are refilled with peptidoglycan and close back up to make the new cells.
Penicillin is able to latch onto the open peptidoglycan during this process and disrupt the filling in of the hole, preventing the bacteria from closing its wall and completing cell division. This creates altering pressure between the inside of the wall and the surrounding fluid and the bacteria cells in effect, burst. If the cells do not immediately burst, the bacteria cells will continue to grow without dividing or developing new cell wall, the wall gets weaker, and eventually ruptures (lysis).
Other antibiotics work by inhibiting the protein synthesis or nucleic acid synthesis. Tetracycline is a bacteriostatic antibiotic that binds to ribosomes in bacteria, preventing the cell from making proteins and stunting further growth.
Consideration must be made when choosing antibiotics to treat diseases as bacteria have a different type of ribosome (70S) to humans (80S), and will only work to target the bacteria. Narrow spectrum antibiotics target specific reaction in particular microorganisms; whereas broad spectrum antibiotics will have an effect on more general features affecting a wide range of pathogens.
Antibiotic Resistance
Antibiotic overuse has led to increasing amounts of bacteria resistant to antibiotics. Antibiotic resistance arises as a result of natural selection. Since bacteria reproduce rapidly, resistance can arise quickly. Those antibiotics resistant will remain after treatment and can continue to divide. Antibiotics have revolutionized medicine and saved many many lives, but bacteria is smart and have evolved becoming resistant to antibiotics.
There are three reasons for antibiotic resistance.
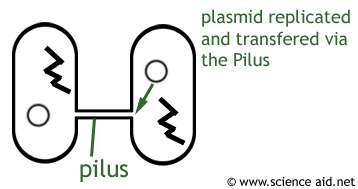
- 1Some bacteria are able to create enzymes that are capable of breaking down the antibiotic. The best example of this resistance is penicillinases. These are enzymes that break down penicillin. This mutated bacteria can spread resistance genes between each other by bacterial conjugation where two cells join by their pilli and exchange plasmids which often contain genes for antibiotic resistance.Antibiotic Breakdown.Advertisement
- 2Some bacteria have advanced to include pump systems that are able to export antibiotics.Antibiotic Removal.
- 3Bacteria that is resistant to antibiotics have mutated peptidoglycan that is less permeable to antibiotics, disallowing the antibiotic to enter.Altered Bacterial Structure.
These three types of mutation are responsible for antibiotic resistance which can be further explained broken down further:
1. Bacteria can undergo mutation (change in structure or form), and when a mutation occurs:
- a. Bacteria can produce chemicals that inactivate the antibiotic. The antibiotic in unable to properly function and get rid of that bacteria.
- b. Bacteria can undergo a gene mutation where the specific target on which the antibiotic binds is modified. The antibiotic can not recognize and bind its target. Think about the lock on a door, when you change the lock of the door, the same key that was used to open the door will not be able to do its job. This is similar to what happens during bacterial gene mutation. The gene changes and the antibiotic that previously may have worked to eradicate the bacteria are unable to eradicate the mutation.
- c. Mutated bacteria can block the hole where antibiotics enter the cell, preventing them from entering.
- d. Some bacteria can also act like a pump pushing out the antibiotics that have penetrated the cell before being able to do their job.
2. Bacteria can obtain antibiotic resistance from another bacteria or virus. For example, when a bacteria conjugates (joins or mates) with another bacteria or virus, then the chemical form of the bacteria changes or one of its receptors are altered prohibiting the entry of the antibiotic to the target cell.
Antibiotic resistance is made much worse by the overuse of antibiotics in medical treatment. Some bacteria are resistant to most antibiotics (MRSA or mycobacterium-tuberculosis) meaning it is increasingly difficult to treat infection unless new antibiotics are developed.
Questions and Answers
I want to work on effect of antibiotics on microorganism in microgravity?
I need assistance on how to run this experiment
It has been proved during space flights and simulations that microgravity not only reduces the effects of antibiotics, but it also affects the development of bacteria. The following link will show you how an experiment sponsored by NASA was conducted; you may use it as an example. Principal Investigator David M. Klaus, Ph.D., BioServe Space Technologies, Boulder, CO, United States
If you want to learn more about microgravity and its effect on antibiotics, I suggest this academic article about the effects of antibiotics during a space flight published by David M. Klaus and Heather N. Howard This other link will take you to an example of how NASA simulated a microgravity environment to study antibiotic production, [http://link.springer.com/article/10.1038%2Fsj.jim.2900345?LI=true Fang, A., Pierson, D., Mishra, S. et al.] These two articles are academic investigations, so you will have to pay to get the full document.
Explain the roles of NAD in anaerobic respiration and describe oxidative phosphorylation in the mitochondrion?
In both plants and animals.please also compare with aerobic respire-aspiration and note any differences
Although those are very specific questions, you can find detailed information in the following links. This article by Eva Biegel and Volker Müller explains NAD in anaerobic respiration. You can also read this one about oxidative phosphorylation in isolated mitochondria from human skeletal muscle by M. Tonkonogi and K.Sahlin. And to complete your search, you can read this article about oxidative phosphorylation by plant mitochondria written by James Bonner and Adelle Millerd.
Referencing this Article
If you need to reference this article in your work, you can copy-paste the following depending on your required format:
APA (American Psychological Association)
Antibiotics: Function, Bacterial Interaction & Antibiotic Resistance. (2017). In ScienceAid. Retrieved Apr 19, 2024, from https://scienceaid.net/biology/micro/antibiotics.html
MLA (Modern Language Association) "Antibiotics: Function, Bacterial Interaction & Antibiotic Resistance." ScienceAid, scienceaid.net/biology/micro/antibiotics.html Accessed 19 Apr 2024.
Chicago / Turabian ScienceAid.net. "Antibiotics: Function, Bacterial Interaction & Antibiotic Resistance." Accessed Apr 19, 2024. https://scienceaid.net/biology/micro/antibiotics.html.
If you have problems with any of the steps in this article, please ask a question for more help, or post in the comments section below.
Comments
Article Info
Categories : Micro
Recent edits by: SarMal, Sim, Jen Moreau